Millions could have helped downtown Fresno hospital. The money went to Clovis instead

READ MORE
Care & Conflict: CMC’s money moves
Click the arrow below for more coverage of Community Medical Centers’ expansion of its affluent Clovis campus.
Expand All
Over the past decade, Community Medical Centers has taken state and federal money intended to offset the cost of providing care for indigent patients, primarily in downtown Fresno, and used it to help fund a $1 billion hospital expansion in affluent Clovis.
How much money is unclear. CMC officials confirmed the use of the funds but refused to publicly disclose the amount when asked by The Fresno Bee.
What is known is that the hospital board’s decision to fund the Clovis expansion happened despite what many consider needed upgrades to its aging downtown Fresno hospital. The hospital needs an estimated $2 billion in repairs to comply with earthquake requirements that threaten the closure of 90% of its acute health care beds.
That is a potentially devastating blow to the region’s poorest patients. In other words, the very people that taxpayer money was intended to serve.
Hospital officials insist that their actions have not had a negative effect on patient care in downtown Fresno. They also contend that the move was financially prudent — building in Clovis is cheaper and necessary because of growth — and that investing in the Clovis hospital still creates an overall benefit for patients in the region.
To be clear, there is nothing illegal about the decision. The state and federal money does not flow to the hospital where the patients generated the revenue, but rather to the operator — in this case, CMC — which has great discretion over how those funds are spent.
That said, advocates and ethics experts told The Bee that the arrangement is beyond troubling and speaks loudly to the inequity of providing health care — an inequity that is exacerbated when hospital corporations prioritize shiny new amenities in affluent communities as a strategy to attract more lucrative insured patients over needed improvements that serve costly indigent patients.
Of greatest concern: Some of the downtown campus’ aging buildings are out of compliance with seismic requirements that now threaten the hospital’s license if major retrofitting isn’t done by a looming 2030 deadline. There is an urgent effort by the California Hospital Association to push state lawmakers to extend that deadline.
Fresno Councilmember Miguel Arias, whose district covers the downtown Fresno hospital, said the situation is yet another example of people in Fresno paying a price to benefit those in Clovis.
“I am disgusted by the idea that they’re using money meant for poor people to subsidize state-of-the-art facilities for suburbs,” Arias said.
BEHIND THE STORY
MOREHow we reported this story
Over the course of roughly two years, The Fresno Bee met with dozens of sources and conducted interviews with current and former Community Medical Centers board members, local healthcare officials, current and former CMC administrators, state and federal agencies, local and state elected officials, and experts on such topics as healthcare, nonprofit organizations and ethical considerations such as conflicts of interest. We made dozens of public records requests and requested data from the state and federal governments. We reviewed property transaction records at the Fresno County Assessor’s and Clerk-Records’s offices. We also reviewed CMC news releases.
The entity responsible for spending the money in Clovis is CMC’s 15-member board, but multiple sources told The Bee the strategy was orchestrated by two people: landowner, developer and pistachio magnate Farid Assemi, who is the current board chair, and former board member Flo Dunn, who was Assemi’s banker and continues to sit in on board meetings as a guest.
Assemi told The Bee in an interview that questions about the funding decision and construction strategy at the Clovis campus should be directed to CMC administration.
CMC, which recently changed its name to Community Health System but is still widely known by its former name, is the area’s largest health care provider. The nonprofit operates four medical facilities: Fresno Heart and Surgical Hospital, Community Behavioral Health Center, Clovis Community Medical Center and Community Regional Medical Center in downtown Fresno, which is by far its largest provider. It employs more than 9,000 workers with an annual budget of nearly $2 billion.

CMC spokeswoman Michelle Von Tersch would not provide specific details about the use of state and federal funding, including how much has been spent on the Clovis expansion. Hospital officials also refused to make public board meeting minutes and other documents, preferring to operate in secrecy. Von Tersch adamantly defended the board’s decisions.
“Community has consistently shared information to reinforce that we follow proper business practices, comply with regulatory requirements and carefully invest our nonprofit resources in a way that supports the health needs of our community,” Von Tersch said in written responses.
There are conflicting narratives about the impetus and motivation for the decision to use money that could have shored up the downtown Fresno hospital, including making seismic improvements, and instead devote it to the Clovis expansion.
Dunn, who was a CMC board member at the time, said the board discussed the expansion project in Clovis after presentations were made by management.
“The project in Clovis,” Dunn said, “was a recommendation from management to our board.”
Other insiders suggested to The Bee a more nefarious motive. The expansion of the Clovis campus has bolstered the development of a nearby pharmacy and osteopathic medical school — the for-profit California Health Sciences University.
The for-profit university was created by and continues to be owned by Dunn and Assemi, the current CMC board chairman.
In addition, the expansion has provided development opportunities for a board member who owns property near the hospital.
“I think this is going to get worse before it gets better in terms of the conflict of interest,” Dr. Ren Imai, a former CMC board member who resigned in 2020, told The Bee. “They are using public funds that should be helping their community to help themselves financially.”
The state of downtown Fresno’s hospital
If there is debate over the motive, there is none over the consequences that have befallen the downtown Fresno hospital — the only Level I trauma center between Los Angeles and Sacramento.
Its most critical patient towers — which house nearly 90% of CRMC’s beds — are more than 50 years old and are showing their age. Patients complain that the rooms are dated, dilapidated and dirty. In addition, the facility has drawn the attention of Fresno fire inspectors, who have cited the hospital repeatedly for code violations.
The hospital also has a potentially larger problem. The 1950s- and 1960s-era buildings are out of compliance with California’s seismic requirements. They either must be retrofitted or rebuilt so they can withstand a major earthquake. If that doesn’t happen and the deteriorating buildings continue to operate, the hospital’s license is in jeopardy.

The current deadline is 2030, but that could be pushed back. Even so, the requirements would remain in place — and the cost of complying with those requirements almost certainly will increase over time.
Andrew DiLuccia, a spokesman for the state’s Department of Health Care Access and Information, formerly known as the Office of Statewide Health Planning and Development, said facilities that are out of seismic compliance would be forced to stop providing services. If that were to happen, it would force patients who may not have transportation to seek care elsewhere.
CMC’s former Chief Executive Officer Tim Joslin in a 2019 letter informed state officials that the CMC board was well aware of its seismic compliance issue.

CMC officials are banking on the extension, but the estimated cost to retrofit is already $2 billion and growing. And the buildings at the downtown Fresno hospital aren’t getting any younger.
“We are really putting a lot of eggs in the basket of getting the state to recognize they are going to have to help us,” said Craig Castro, CMC’s chief executive officer.
Some would argue that help was already available — in the form of the state and federal money CMC instead chose to spend on the Clovis expansion.
Fresno Councilmembers Arias and Esmeralda Soria urged hospital officials to stop pursuing an exemption and focus on a financing plan.
“I told them that any state agency that would consider an exemption for earthquake standards was playing Russian roulette with the lives of Fresnans,” Arias said, “and that they should stop advocating that path, and instead finance the construction of the tower because they have plenty of capital and borrowing capacity to build the facility.”
But Castro said CMC plans to wait and see how their requirements are going to play out.
“Seismic,” he said, “is informing our future investments downtown.”
The state and federal money in question
The funding in question is the hospital’s payout from the state Hospital Quality Assurance Fee program. That money compensates CMC for its care of poor and underinsured patients. The ratio of these patients seen at the downtown hospital compared with the Clovis hospital is 6:1. Because the lion’s share of these reimbursements were generated by patients served at the downtown hospital, much of the money rightfully might have gone to its renovation and expansion.
Nancy Hollingsworth, president and chief executive officer of Saint Agnes Medical Center in Fresno, believes that’s the decision CMC’s board should have made.
“These fees are intended to be used to bolster the programs and services that benefit our community’s most vulnerable patients and should be reinvested in the programs and services at the location where they were generated and most needed,” she told The Bee. “As taxpayers, we should all be concerned about how not-for-profit hospitals are using provider fee payments.”
Instead, CMC’s board voted to underwrite the Clovis expansion.
It was financially prudent, Castro explained, to build in Clovis — and hope the state helps solve the seismic crisis.
But what if no deal can be made with the state? Is it possible the hospital could lose its license at some point in the future? Could the hospital even be shut down — or at least some portion of it? That would seem inconceivable, but it’s still the very real fear of many.
Assemblyman Joaquin Arambula, D-Fresno, a physician, said CMC should have planned better, especially because of its trauma hospital status.
“We must be prepared for any huge emergencies, including earthquakes, that will happen,” he said in a statement to The Bee.
The hospital, he said, cares for many poor and disadvantaged residents who seek services there. “We must ensure that it is protected and keeps its doors open,” he said. “If not, the consequences will deliver a devastating blow to health care in our entire San Joaquin Valley.”
Seeking further help from the state
Von Tersch, the CMC spokeswoman, stressed that the corporation “completed substantial design work on bed replacement” in 2016-17, but it appears that “design work” is as far as the effort has gone. Once the hospital realized the necessary renovations would cost more than $2 billion, Von Tersch said the hospital instead shifted its focus to working with the state hospital association on legislative relief.
Von Tersch also stressed that this is not just a problem in Fresno and that 63% of California hospitals “won’t meet the 2030 seismic regulations.”
But when contacted by The Bee, the state provided a much different perspective:
According to the state’s Department of Health Care Access and Information, 2,443 out of 3,160, or 77.3%, of general acute care hospital buildings on 416 hospital campuses across the state meet the 2030 seismic requirements.
Other hospitals in California, such as Enloe Medical Center in Chico and Marshall Medical Center in Placerville, find themselves in similar situations as Fresno’s downtown hospital and the fate it faces with the 2030 deadline. A clear distinction, however, is that these two hospitals — which are also not-for-profit entities, just like CMC — have been planning and setting aside money for years to address their seismic issues.
Officials at Enloe and Marshall medical centers, just like Von Tersch, described the seismic requirements as massive “unfunded mandates” from the state that have been challenging and will require sacrifices and compromises. Still, both hospitals have been actively working to renovate facilities and build new expansions to be in compliance whenever that deadline comes around.
Bill Seguine, director of facilities at Enloe Medical Center, said the hospital in 2012 completed a major $175 million construction project to add bed capacity to the original hospital. More recently, he said, it also upgraded one of its other buildings to come into compliance.
“The bottom line from Enloe’s standpoint is, yes, we know how to comply, we know how to make these things work — these are the rules that we have to play by,” he told The Bee during an interview. “At the same time, this is a massive, massive cost and where the dollars for all these costs come from without sacrificing quality and patient access to care, we don’t know.”
Siri Nelson, chief executive officer for Marshall Medical Center, said there are high stakes with being a community nonprofit hospital.
“We have to be very careful about how we spend our cash,” she told The Bee during an interview. “I’ll just share the famous quote from ‘Spider-Man’: With great power comes great responsibility.”
With that said, Nelson said that as the hospital has done renovation projects, it has approached them in a way for those upgrades to meet seismic standards for 2030.
In 2014, Marshall Medical Center completed an expansion — the south wing — that now houses the emergency room, the intensive care unit, the OB unit, the kitchen and the cafeteria. That expansion is seismically compliant, she said, and hospital officials are trying to maximize the capacity of that addition ahead of the state’s deadline.
Seguine believes most hospitals will be able to come into compliance by the deadline, but that’s because many “hospitals are part of hospital systems, and those systems have a lot of more money and resources behind them.”
Fresno’s downtown hospital is part of a hospital system that has money and resources, yet it faces a similar fate as small, rural hospitals if it remains out of compliance.
Dr. James Davis, the chief of trauma and surgery at the downtown Fresno hospital, said the community would suffer if the flagship campus lost its license.
“It would be a disaster for critical illness and injury. It would be a disaster because there wouldn’t be a safety net hospital, and people who need care but don’t have other avenues, or access to care, wouldn’t get it,” he told The Bee. “It would be awful.”
Poor patients, who often lack transportation, essentially would lose access to the downtown hospital, and would be forced to travel to the Clovis campus — 12 miles away — seek services elsewhere or go without medical care.
The impact in human terms
Carlota Espinoza is one of those patients.
On a recent afternoon, Lorena Espinoza pushed her elderly mother, Carlota, in a wheelchair from the downtown hospital on their way to a parking garage. Her mother, who has Medicare, had just undergone an MRI for a spot detected on one of her lungs.
“My main concern would be what happens to all the patients who come here because both my parents are elderly, and all their appointments are either here or at the other clinic (in Fresno),” the adult daughter said. “What happens to patients that could only use Medi-Cal or Medicare? .... I’m speaking for the majority, what happens to the people, the majority who don’t have private care?”
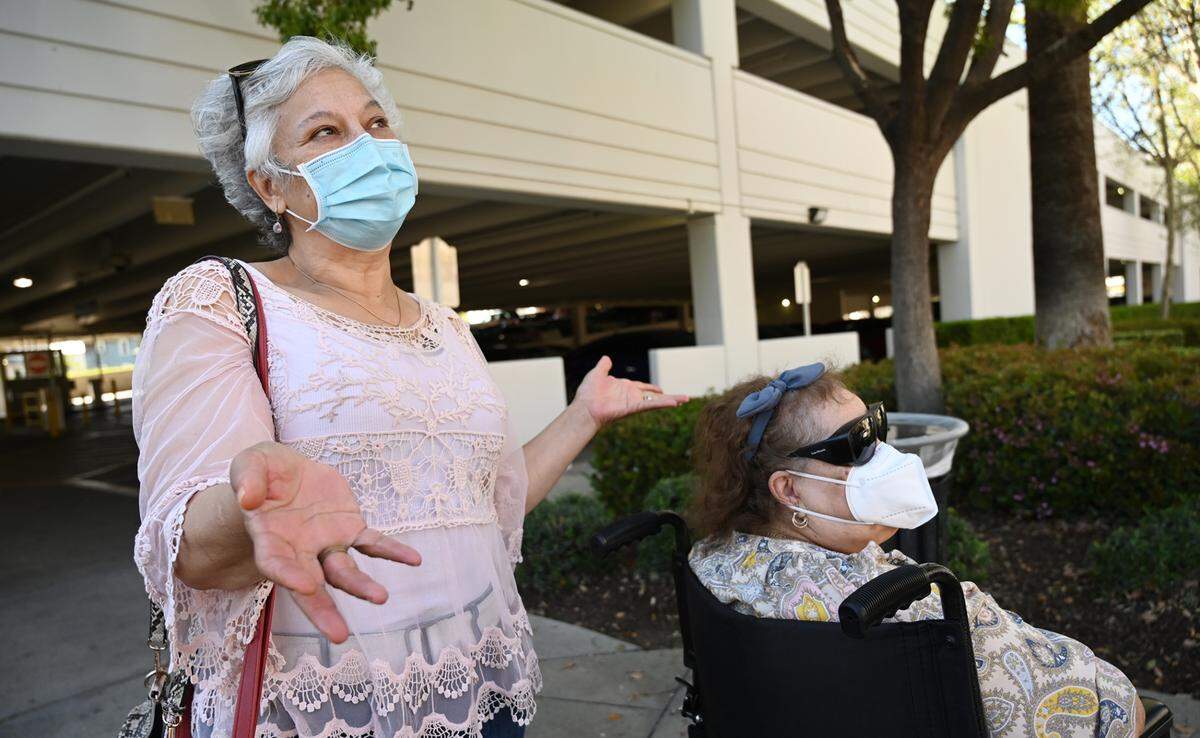
Lorena Espinoza now lives in Monterey but comes to Fresno to take her parents to their medical appointments. She has siblings who live in Fresno and in Clovis.
About 12 years ago, Lorena Espinoza said she first noticed the Clovis campus began to expand, and yet, CRMC hadn’t even seen improvements in its interior rooms — “it still looks the same.”
She was shocked to learn state and federal funding generated at CRMC had been used for the expansion of the Clovis campus.
“Now that I know that, it makes me upset because, you know what, it really does. It just shows how the majority of the money always goes to the wealthy, and Clovis is a wealthy community,” she said. “I’m very concerned, and it really upsets me. If anything, they should be pumping more money and utilizing it where they give the most care.”
The Clovis hospital, Councilmember Arias said, “is meant to serve ... the elective surgeries of one of the richest suburbs in the state at the expense of the poorest people in the state.”
Most patients who go to the Clovis campus have private health insurance and are able to pay for their care.
As medical services move away from downtown — an area with great need — to Clovis, researchers at Johns Hopkins University, analyzing inpatient and outpatient Medicare claims, recently found the Clovis hospital to be among 20 health care facilities in the country that provide the most “unnecessary” care. The Medicare claims examined were from 2015 through 2018, and researchers identified 17 low-value medical services and identified the number of patients who were eligible for those services, and then those who received the service.
A spokesperson for the Centers for Medicare & Medicaid Services referred questions from The Bee about the use of federal funding by CMC to the California Department of Health Care Services.
“The Hospital Quality Assurance Fee (HQAF) program is a California state-run program, not a federal program,” the spokesperson said in an email.
The federal government, however, provides matching funds.
“There is no requirement on how these funds are to be spent,” said Anthony Cava, a spokesman for the California Department of Health Care Services (DHCS).
When asked if officials saw the use of these funds by CMC as appropriate, Cava said the department’s hands are tied because it doesn’t “have the authority to direct how those funds are used by community hospital systems.”
The CMC board has viewed this as free rein to send the money where it pleases.
And it’s a significant pool of money.
For fiscal year 2021-22 alone, the downtown hospital is estimated to have generated $128.1 million in payments from the same fee program. In comparison, the Clovis hospital is estimated to have generated only $22.4 million.
To understand just what a vital economic and health care engine the downtown hospital is, consider the government funds it generates — reimbursements that go into the coffers of the entire CMC network. In the past decade, the downtown hospital brought in more than a billion from the Hospital Quality Assurance Fee program, according to California Department of Health Care Services figures requested by The Bee. In comparison, the Clovis hospital brought in around $150 million.
“The money is viewed as a system asset, and we’re looking to serve the region,” Castro, CMC’s chief executive officer, said in an interview with The Bee. “The money that came from the government was in order to support the patients we care for as a system, and we used it in the best way, as a system, to get the most capacity.”
Joan Harrington, director of social sector ethics at Santa Clara University School of Law’s Markkula Center for Applied Ethics, said there’s no legal question about CMC spending the state and federal money in Clovis. However, it’s still problematic.
“I believe there is an ethical issue about allowing one of their hospitals to sort of languish and potentially be closed because of a failure to bring it into earthquake compliance,” she said. “I think it’s questionable whether the decision to put most of the money into Clovis was an ethical decision.”
Harrington said perhaps the law should be reviewed.
“It would be worth revisiting the reasoning behind this flexibility,” she said, “when the funds are intended to compensate a particular hospital for treating the poor.”
State lawmakers could indeed draft legislation that limits how — and where — the money is spent.
The state Legislature, however, isn’t the only government authority that could take action. The Fresno City Council might also have some leverage.
Was the agreement fulfilled?
In 1995, CMC entered into an agreement with the city of Fresno to develop the CRMC campus in exchange for land the city gave the hospital. There is disagreement between the city and CMC about whether that agreement has been fulfilled.
Fresno council members — having watched money be directed to Clovis — have put CMC on notice. They have requested that the hospital develop a financing plan to build at least one new tower at the downtown hospital.
“What I think (is) going to happen is,” Arias said, “it’s going to force the city of Fresno to consider all our legal options in holding (CMC) to their commitment to build a tower there and to complete the rest of the campus there.”
It’s not the first time that health care services have been shifted out of Fresno. In 1998, Valley Children’s Hospital was moved to southern Madera County. CMC also has purchased more than 200 acres in Madera County with plans to build a hospital there — the “next Clovis,” as Castro calls it.
Arias is also troubled because he said that he and Councilmember Soria, when questioning the new towers in Clovis, were initially told in late 2020 that they were built with donations, not funds intended to supplement care for indigent patients.
Von Tersch told The Bee that CMC met the 1995 agreement when it built “the trauma and critical care building and the East Medical Center Plaza and medical offices.”
CMC had planned in 2002 to replace the aging West and East wings at its downtown campus, records obtained by The Bee through a public records act request show. The hospital’s acute care services were to be relocated from the East and West wings to new towers. CMC envisioned building two new towers as part of the hospital’s 2030 seismic compliance plan. The records, submitted by the hospital to state regulators, show CMC had hoped to complete the first tower by 2010 and the second tower by 2020.
The hospital, however, seems to have moved away from its strategy to build the new towers at CRMC sometime after 2006. That was after it successfully requested a delay in seismic compliance for what was then a looming 2008 deadline, saying if it had to close the West Wing and another building, it “would result in diminished health care capacity for Fresno County.”
A kingdom in Clovis
The board eventually would shift its attention to a new strategy: A massive expansion in Clovis.
It was a move that not only put off spending money to retrofit the downtown Fresno hospital, but the decision was also potentially more beneficial to Assemi, Dunn and some members of the board.
Assemi and Dunn wanted to build a for-profit medical school — and the proximity and partnership opportunities of building it next to a hospital they had some control over would increase the likelihood for success.
Not surprising to some, the board began focusing much more attention on the Clovis campus. In 2010, construction began on the first new tower in Clovis. In 2011, it moved its administrative headquarters to a new building in Clovis, despite the hospital corporation’s bylaws specifying its principal office must be located in Fresno.

In 2012, the same year Assemi and Dunn’s for-profit school was launched, the CMC board approved the construction of a 25,000-square-foot Clovis Health and Education Conference Center at the Clovis hospital. At the time, CMC announced the center would help “provide health education.” The center was completed in 2013, according to Clark Construction, which worked on the project.
Over time, CMC began moving critical medical services to its Clovis campus.
The hospital corporation developed a new endoscopy center at the Clovis campus, and it has the only Level 3 fertility center between Los Angeles and Sacramento.
While the flagship downtown hospital offers some cancer services, CMC decided to locate its cutting-edge, comprehensive Community Cancer Institute in Clovis. The state-of-the-art facility opened in 2018, and on its website, CMC compares the institute to cancer centers in Los Angeles and the Bay Area.
And CMC will consolidate heart medical services at the Clovis campus, “so that the heart hospital can be used for other purposes,” Castro said. He said he has strategically planned the consolidation, but didn’t want to go into details at this time.
“We are going to see this become the hub for heart,” Castro told The Bee.
Open-heart surgeries will still be available at the downtown hospital for patients who “helicopter in,” he said.
Then, in 2018, came the most significant development: The board approved a second, $390 million tower.
By the time Arias and Soria met with CMC officials in 2020 — in those new Clovis headquarters — Arias said the situation had become transparent.

“I came away from that meeting with a clear understanding that the hospital had made an intentional decision to move away from what Fresno has experienced, as you know, a community benefit hospital to a more private health care system,” Arias said of the meeting in the fall of 2020.
Von Tersch maintains that the Clovis expansion project was not motivated by the financial interests of board members. She said the decision in 2007 simply reflected population growth in Clovis. Further, Castro said it was more cost-effective to build in Clovis.
And almost certainly more beneficial to CMC’s bottom line; money spent to retrofit the Fresno hospital would not help the balance sheet in the same way that investing money in Clovis would, where all those amenities could attract private-insured patients.
But some question whether it was only the hospital’s bottom line being considered.
A new medical college
Insiders have told The Bee that Dunn and Assemi have played outsized roles in steering the board’s expansion ambitions. Dunn was a board member at the time and recruited Assemi around 2006, first to join a committee and then to be a full board member in 2009.
At the time, Assemi told The Bee, Dunn had told him his area of expertise was finances, and the hospital system was anticipating a “billion dollars worth of construction projects.”
Von Tersch notes that “the decision to expand this campus was made prior to Farid Assemi joining our Board of Trustees (2009) and prior to the founding of California Health Sciences University (2012).”
But Assemi’s involvement with the board seems to have pre-dated or coincided with the expansion decision. And Dunn’s and Assemi’s vision to build a for-profit medical college was made long before 2012.
The first major expansion project in Clovis began in 2010 — a year after Assemi joined the full board. Significant construction projects continued there for the next decade, including the bulk of the Clovis expansion.

The Assemi family pitched the idea for the current site for CHSU in late 2016. Two years later, the CMC board approved the second tower at Clovis Community Medical Center. The osteopathic college — also owned by Assemi and Dunn — was then built less than a mile from the ever-expanding Clovis hospital campus.
When asked by The Bee whether his ownership of the for-profit school influenced the board’s expansion efforts, Assemi issued this statement:
“As with all nonprofit boards, Community’s board recognizes its obligation to assure compliant business practices. This includes adhering to a policy on conflict of interest, which is based on federal and state laws. I have personally adhered to that policy throughout my tenure on the board. I am confident that my fellow board members and Community’s management know that first and foremost my actions have sought to advance our mission to serve the people of our Valley to the best of our ability.”
What might have been
Sandra Celedon, chief executive officer of Building Healthy Communities in Fresno, said that at one time, CMC seemed sincere about its intention to be an anchor in downtown Fresno.
“I would say that maybe about a decade ago, the conversation shifted to think more about building a kingdom as opposed to building health infrastructure,” she told The Bee.
And that kingdom would be in Clovis.
While the new trauma center was completed at the downtown facility, the towers were never built. Instead, CMC announced in July 2010 that it had reached a “milestone:” The last steel beam on a new five-story tower was put in place at the Clovis hospital. The tower was part of a $320 million expansion that was completed in 2014 and nearly doubled the Clovis hospital’s capacity. Soon after came a $68 million cancer center, a $390 million second five-story patient tower, and a $65 million skilled nursing facility that has been paused now. The second tower at the Clovis campus is expected to be completed this year.

Advocates for the downtown Fresno hospital see inequity in that investment in Clovis. But CMC officials insist improvements have been made in Fresno, as well.
Von Tersch, as well as Brianne L. Marriott, CMC’s chief legal counsel, said that CMC has invested $500 million in the downtown hospital, dating back 15 years. The largest project was the new trauma center, which Marriott noted cost $200 million. That was completed in 2011 and was one piece of the hospital’s 2030 seismic compliance plan, which, of course, remains significantly unfinished.
Marriott pointed to other, lesser improvements during the past 10 years, including an office building for outpatient specialty care, an ambulatory care center, a new central energy plant and two parking garages.
Marriott, in a letter to The Bee, said the downtown hospital buildings were in ”excellent condition” and that they meet “all current applicable standards.”
Kathryn Peisert, managing editor at The Governance Institute, which supports health care boards to lead stronger organizations, said it’s a “huge concern” that CMC decided to fund new towers in Clovis instead of retrofitting the Fresno location.
“At the end of the day, it’s like, ‘are we doing the right thing for our patients and the communities that we serve?’” she asked. “It’s very hard to see that was the mindset of the people making these decisions.”
For Arias, the fate of CMRC is personal. The downtown hospital is where he took his mom when she had a brain tumor and where his daughter was treated when she became ill due to COVID-19.
“It seems to me,” he said, “that CMC is losing its founding principles to treat the poor and to provide the best care possible to those who need it the most when they have the least.”
If so, the consequences of that decision — spending money on the Clovis hospital instead of downtown Fresno — Celedon believes, will be dire.
When hospital systems move away from vulnerable communities, she said, and residents struggle to access medical care, “folks end up dying.”
This story was originally published August 25, 2022 at 5:00 AM.
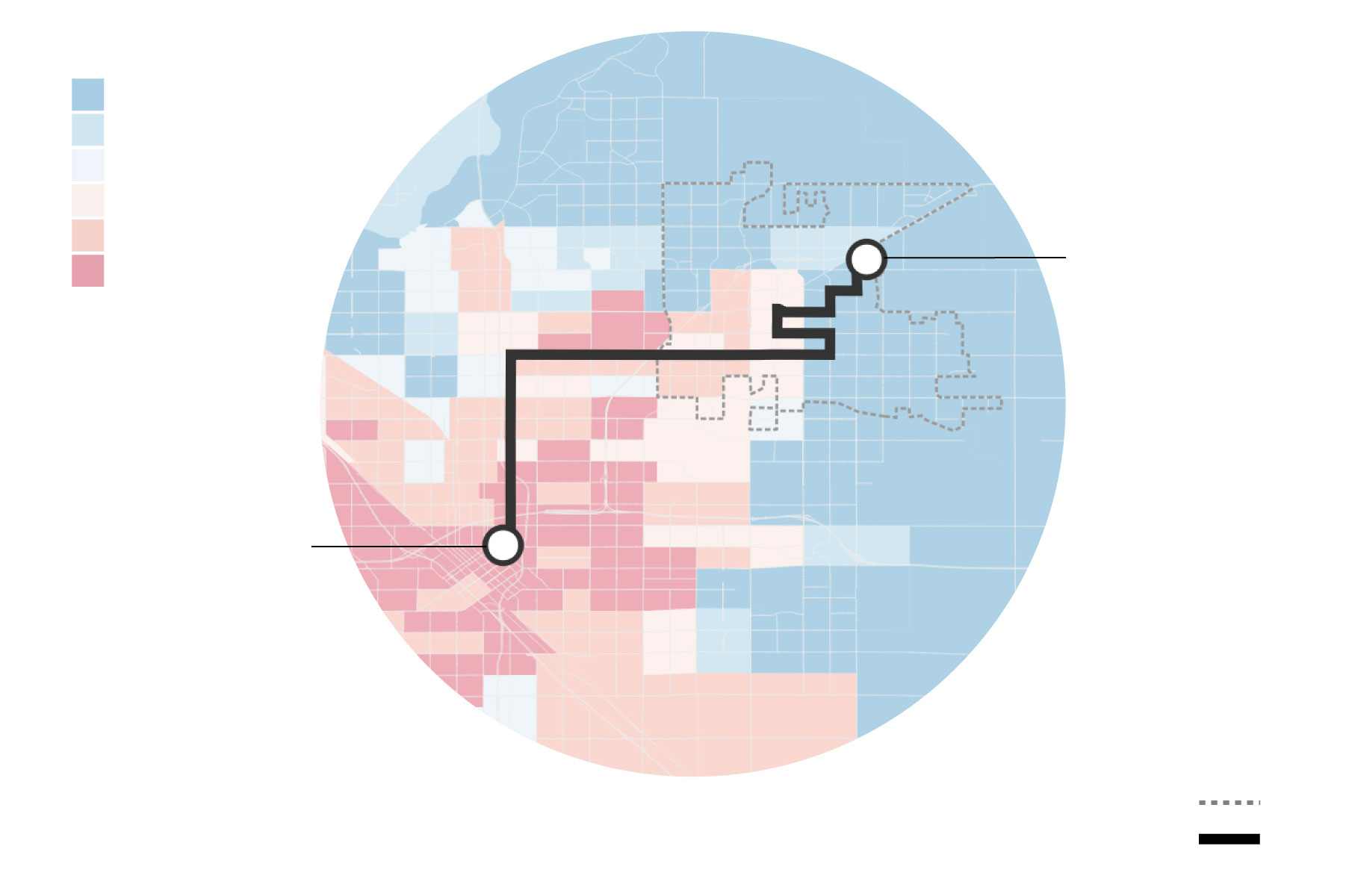
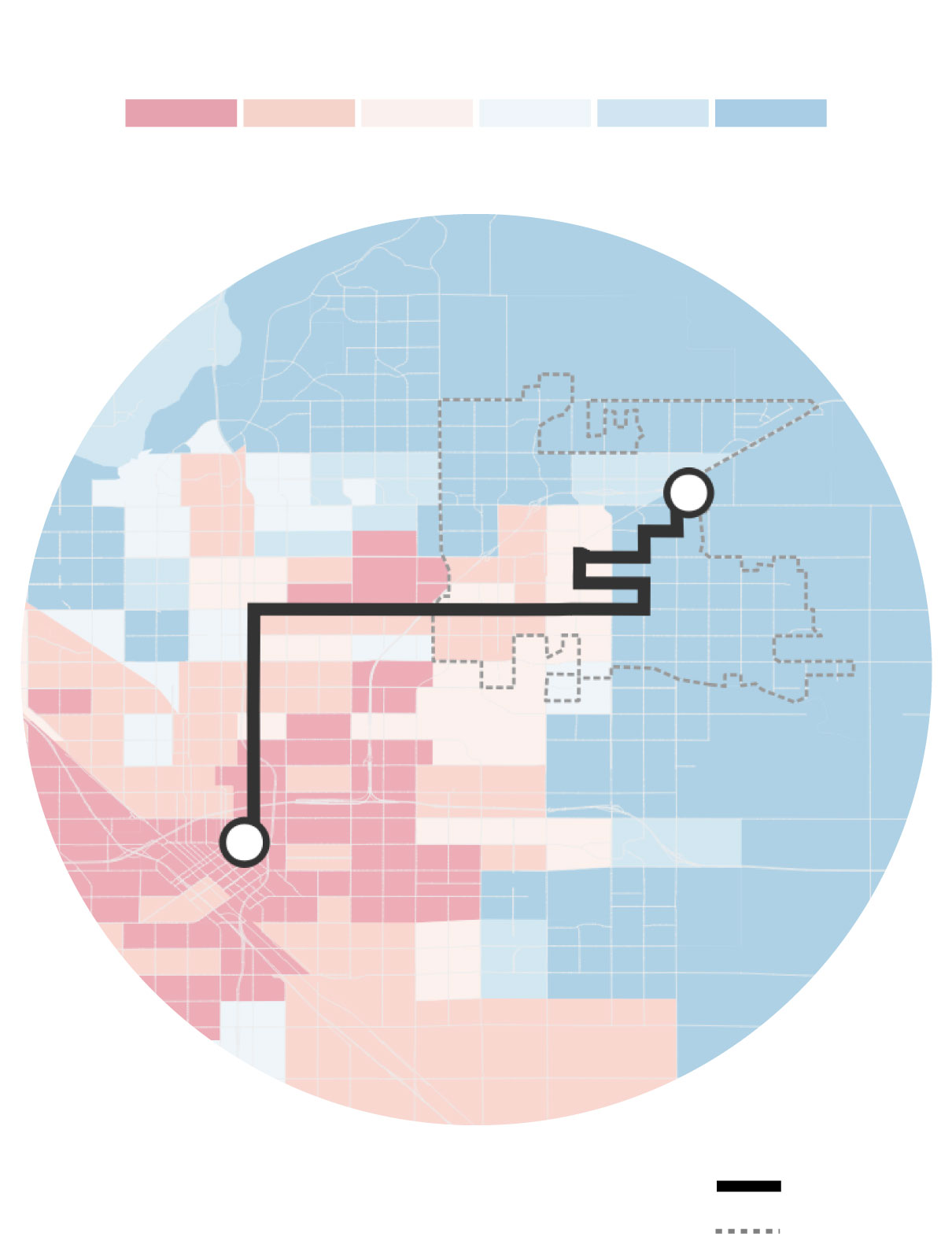
.jpg)





