‘I don’t want you to go.’ Fresno health care workers cry, pray with coronavirus patients
Dr. Elisa Avik has listened to Christmas music on her way to work recently in an attempt to cheer herself up.
Her patients are now relying on her more than ever to raise their spirits as they recover from illness without family members at their sides.
Kaiser Permanente Fresno, where she works, hasn’t allowed visitors to see hospitalized patients over the past month, like other hospitals across the country, in an attempt to reduce the spread of contagious COVID-19. Avik and other health care workers have stepped up to help, taking on new duties including video conference calls with worried family members multiple times a day.
“It’s probably the only bright spot in the day because it’s so stressful,” said the critical care pulmonologist about connecting patients with their families during those calls. “It’s almost like being Santa, to give a little joy.”
But video calls only help so much.
Stephanie Edwards, an assistant nurse manager at the hospital, has had patients grab her hands and beg her not to leave their rooms. Not having families in the hospital — except for a few exceptions, including end-of-life care — has been a big change.
“They are scared,” Edwards said of patients. “I’ve prayed with them and I’ve cried with them.”
Emotional toll on nurses, doctors
Avik and Edwards, both 39, have children at home who are struggling, too. Edwards’ 15-year-old daughter is very worried.
“She’s very bright, very aware of what’s going on,” Edwards said. “She’ll call me at 3 a.m. crying, saying, ‘I don’t want you to go, I heard a nurse died.’ It’s hard.”
There’s been times Edwards has cried in a closet at work to regain her “game face.” One colleague who spotted her in tears insisted on giving her a hug, despite knowing the risk. It was the first hug she’d received in two weeks.
Edwards has been isolating herself at home, staying in a separate room from her husband, another health care worker. It’s an attempt to keep each other and their patients safer. Edwards sees her husband in person when he brings plates of food to her door.
Avik isolated herself at home for two and a half days recently when she was sick and waiting for the results of a coronavirus test, which came back negative. She comes home from work at night and barely sees her 18-month-old son and 4-year-old son, who misses her. She doesn’t take her work shoes home and doesn’t let anyone touch her until she’s showered.
Avik said she’s experienced many different emotions over the past few weeks.
“Being scared, being like angry I guess — angry that we’re in this war against something you can’t see,” Avik said, “and you don’t really know what’s the best treatment for it.”
Rush to meet a growing need
Edwards oversees a 24-bed telemetry unit now devoted solely to COVID-19 patients.
Avik, who specializes in critical respiratory care, works in a 12-bed intensive care unit that’s divided between those under treatment for coronavirus and those who aren’t. Kaiser has a surge overflow plan to increase its Fresno ICU beds to more than 50.
Avik estimates the ICU is about double its normal capacity for this time of the year.
Kaiser and Fresno County public health officials didn’t share how many coronavirus patients have been treated at Kaiser or other area hospitals, including the larger Community Regional Medical Center.
Fresno County had 265 coronavirus cases and a total of seven COVID-19 deaths, as of Wednesday night.
Edwards said coronavirus has placed a greater demand on her hospital than the seasonal flu ever did, and that things are chaotic and ever-changing.
“We’ve never had units full of just flu patients. It’s definitely different,” Edwards said of coronavirus.
Edwards said she’s seen the health of coronavirus patients decline quickly, with patients suddenly needing to be intubated within a matter of hours. Fresno County health officials warned that the Fresno area could need hundreds more ventilators and ICU beds.
“With this virus,” Edwards said, “it’s very clear when it’s taking a turn for the worse.”
Breathing issues aren’t the only big risks.
“It is different in the sense that they do get worse before they get better,” Avik said of coronavirus, “and they develop other organ complications, for example kidney issues, in addition to their breathing failure.”
Protective equipment concerns, nurses get COVID-19
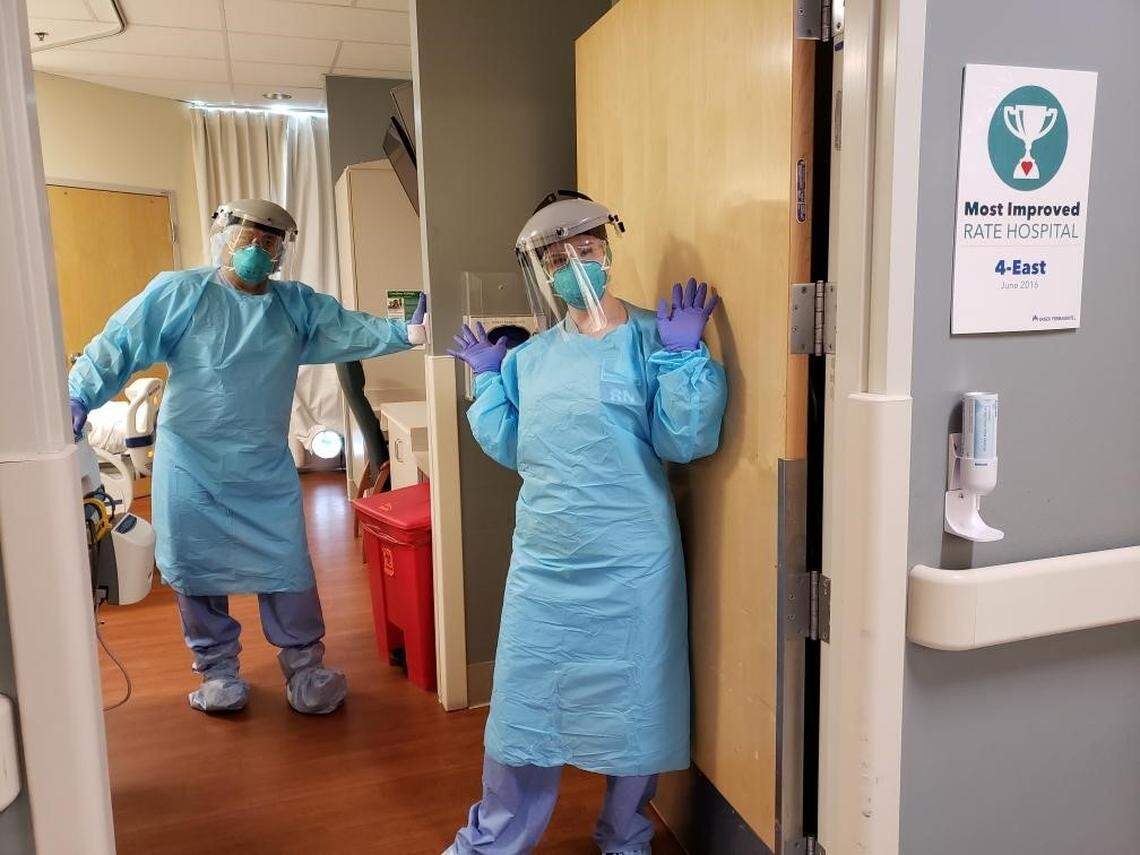
Health care workers are putting on more layers of personal protective equipment in recent weeks.
Edwards said suiting up – including head shields, masks, hospital gowns and gloves – sometimes makes her feel like she’s in the movie “Alien.” Avik compared it to scuba diving, with a buddy who checks to see that equipment is on properly. There are additional guidelines about how to safely remove it.
“But everyone is still scared,” Avik said, “scared of getting infected.”
Patients with coronavirus are being separated from others without it. Avik said this also helps reduce the use of protective equipment. She said gloves are changed and hands washed between patients, but that staff keep the same head shield and mask on.
Some Kaiser workers said the hospital has not done enough to keep employees and patients safe, alleging previous standards for using protective equipment have been thrown “out the window as if they never existed.”
Members of California Nurses Association, National Nurses United held a protest Tuesday outside Kaiser Permanente Fresno, stating nurses there have to reuse the same N95 respirator masks for an entire shift or sometimes longer, opening up the risk of cross-infection, and that management planned to have nurses wear gowns for an entire shift.
The union said dozens of nurses were exposed to COVID-19 – including three now hospitalized, and one in critical care – after a coronavirus patient admitted to the hospital in late March wasn’t tested until days after admittance.
Kaiser leaders called the union’s claims inaccurate, but confirmed 10 nurses at the Fresno facility tested positive for the virus – seven of which were determined to be work-related.
“It is possible for staff to come in contact with patients who are asymptomatic and do not meet the CDC criteria for suspected COVID-19, but whose condition evolves to be suspected for COVID,” said Wade Nogy, senior vice president and area manager of Kaiser Permanente Fresno, in a long statement. “That’s why our staff are provided and wear clinically appropriate masks in patient care settings.”
Caring about patients
Beyond medical care, nurses and doctors are doing little things to help on an emotional level that have meant a lot.
In one case, after Avik learned one of her sedated patients was a music lover who always had a boombox going, she reached out to his daughter to ask about the man’s favorite music. Avik then played that music in his room.
In another instance, Avik videoed a patient walking around the ICU after being bedridden, a joyous occasion she described “like watching his first steps again.”
To help pass the time, patients are given coloring books, playing cards, puzzles and additional phone chargers. Edwards has also been trying to hang out with patients a few minutes longer than she used to.
Patients additionally can chat with nurses via video that’s similar to Facetime, and in an attempt to reduce everyone’s exposure, some staff, including dietitians and social workers, are checking in virtually instead of in-person.
How to help? Stay at home, believe it’s serious
Edwards has heard parties near her home recently and seen driveways loaded with cars. She wishes those people knew how much gatherings contribute to the virus’ spread. She wishes they could see what she sees daily at the hospital.
“They don’t really see the effects.”
Coronavirus patients can be asymptomatic, she said – the ability to pass the contagious virus on without displaying any symptoms.
And for those still comparing the seriousness of COVID-19 to the flu, “I would definitely myth bust that,” Edwards said.
Avik said although many may want to return to normal daily life now, it’s important that people don’t.
“If people revert to the old ways, it will just result in a second surge,” Avik said. “We have to continue the good work we’ve already done.”
Kaiser is not actively collecting medical supplies like some other facilities. It’s part of a larger network of hospitals that can share resources. But the public can still drop off unused supplies near its drive-in testing station outside the hospital, which is for Kaiser members with a doctor’s referral, hospital officials said.
There’s other ways to help health care workers.
Most importantly: Take coronavirus seriously, stay at home, social distance, and practice good hygiene, including frequently washing hands, Edwards said.
“That’s the best way to help us.”
This story was originally published April 16, 2020 at 12:31 PM.
