Study finds troubling connection between wisdom teeth removal and possible opioid use
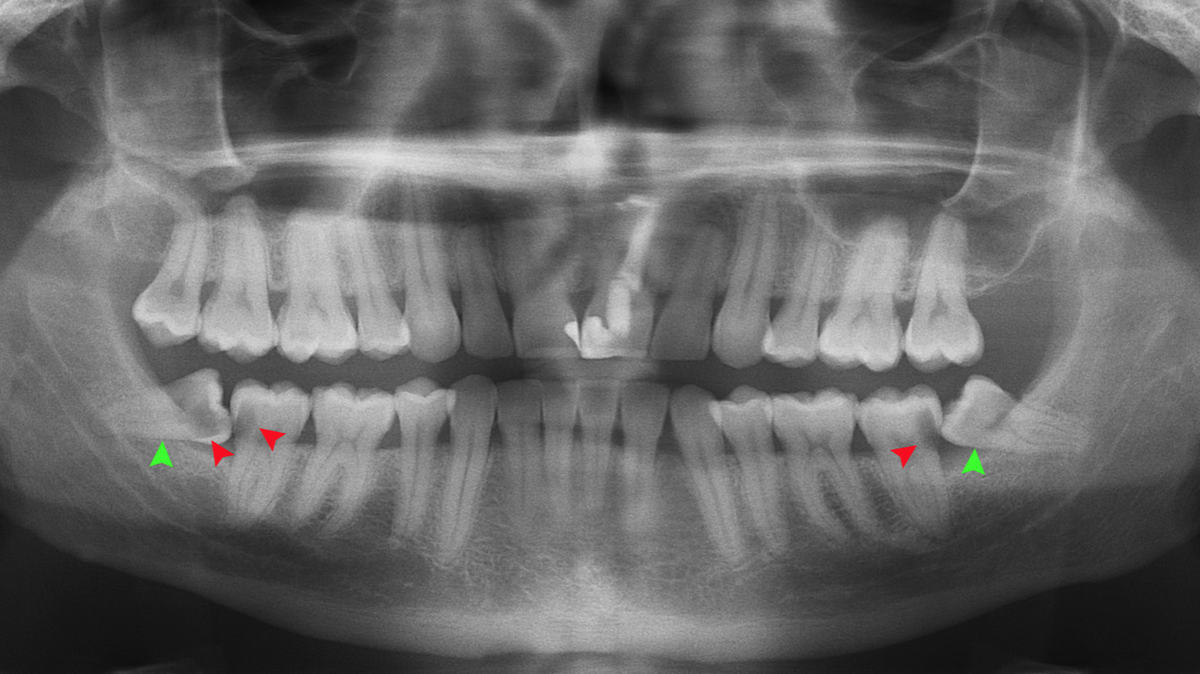
Millions of people each year go through the dreaded experience of getting their wisdom teeth pulled out.
A new study from researchers at the University of Michigan suggests that for some people, the experience could set them up for long-term possible opioid use.
The study, published in the journal JAMA, found that those who were prescribed an opioid for wisdom teeth removal had almost triple the chance of “long-term” possible use of the drug when compared to those who were not given an opioid.
Dr. Calista Harbaugh, the lead researcher of the study, told ABC News that the study suggests medical professionals should consider when — if ever — they should prescribe opioids to patients who just had their wisdom teeth pulled.
“From our findings, we should strongly consider not prescribing any opioids routinely after wisdom teeth are pulled,” she told ABC. “Particularly since there is evidence that anti-inflammatories may be just as good, if not better, for pain management after wisdom teeth are pulled.”
For the study, researchers examined around 71,000 people who had insurance from 2009 to 2015 and also had their wisdom teeth pulled. Those included in the study were 13 to 30, had no prescriptions for opioids up to six months before their wisdom teeth surgery, hadn’t been under anesthesia for a year and hadn’t been through another dental operation in the last year, the study’s authors noted.
Nearly 80 percent — or 56,686 — of people whose wisdom teeth were pulled also filled a prescription for opioids, the study found, while the remaining 14,256 didn’t fill a prescription for the drug.
Yet 1.3 percent of those who filled the prescription later experienced “long-term” possible use of opioids, the study’s authors noted, while the same could be said for just .5 percent of those in the second group.
That means those prescribed opioids were 2.7 times more likely to keep filling prescriptions for the drug, the study found.
Harbaugh explained why those findings are significant.
“Until now, we haven’t had data on the long-term risks of opioid use after wisdom tooth extraction,” she said in a University of Michigan press release. “We now see that a sizable number go on to fill opioid prescriptions long after we would expect they would need for recovery, and the main predictor of persistent use is whether or not they fill that initial prescription.”
One major caveat is the study just examined prescriptions of opioids, and not whether the pills had been taken.
Older teens and younger adults had a heightened risk of receiving opioid prescriptions for a long time, the study noted, especially if they had a chronic condition or a mental illness like depression.
Romesh Nalliah, a dentist who worked on the study, also said that dentists should consider if a wisdom tooth even needs to be extracted at all.
“We hope that our study will make my fellow dentists think twice about removing wisdom teeth,” he said in the press release, “and to more strongly consider non-opioid solutions.”
Others have to started to question whether it’s necessary to remove some people’s wisdom teeth if they don’t cause problems.
A 2014 study found that around 83 percent of people with an impacted wisdom tooth spent a whole year with no symptoms of the problem. And a 2007 in the American Journal of Public Health suggested that only one-third of wisdom teeth removals are actually necessary for a medical condition.
Still, Vox reports that nearly 10 million wisdom teeth are removed in the U.S. each year, costing people nearly $3 billion.
University of North Carolina oral surgeon Dr. Ray White explained that it’s better to act early and get the wisdom teeth out, instead of waiting until they cause a problem later in life.
“You might not have symptoms now,” he told Vox, “but you can’t assume it’s gonna be that way for the rest of your life.”
This story was originally published August 9, 2018 at 8:38 AM with the headline "Study finds troubling connection between wisdom teeth removal and possible opioid use."