Coronavirus updates: Southern California ICU capacity hits 0% as state drops to 3%
Intensive care unit space is scarce and becoming thinner by the day in California, where mountains of new coronavirus cases are also being detected on a daily basis — a distressing sign that an even worse hospital crisis and higher death tolls could be looming in the coming weeks.
The state’s hospital systems are burdened by nearly 15,500 confirmed COVID-19 patients, recently surpassing double the summer peak experienced in July. Almost 3,300 of the current patients are in intensive care, state data show, a record that’s been extended upon every day since breaking it Dec. 2.
Between those with the virus and those requiring critical care for other reasons, ICU availability in the nation’s most populous state stood at just over 3% as of Thursday, down from 4.1% one day earlier, according to the California Department of Public Health.
The state says there is now no remaining capacity in the sprawling Southern California region, home to 20 million people. After days fluctuating to and from 0%, the San Joaquin Valley region of 7 million people had 0.7% as of Thursday.
The Bay Area, which has fared generally well during the pandemic, taking some of the quickest and most restrictive actions to tamp down the virus growth curve, on Wednesday dropped below 15% ICU availability, at 13% by Thursday. That triggered the state’s regional stay-at-home order, which Gov. Gavin Newsom announced earlier this month.
Four of the state’s five geographic regions, combining for 98% of its 40 million residents, are now subject to the order, which directs restaurants to close down both indoor and outdoor dining and prohibits barbershops and salons from operating. Those and a few other restrictions must stay in place for at least three weeks in each region before the state reassesses its ICU situation.
Greater Sacramento, made up of 13 counties clustered near the state’s capital and the neighboring foothills, had hovered near but mostly slightly underneath the 15% mark since first dropping beneath it on Dec. 9. It’s now at just over 11%.
Only Northern California, the least populous of the regions by far, had more than 15% ICU availability as of Thursday, at 26%.
Hospitalizations for COVID-19 are growing exponentially, in conjunction with booming infection rates statewide. And, with the most direct correlation to ICU cases, deaths from the disease are coming at their fastest clip yet in California. An average of 173 deaths a day have been reported over the past two weeks, flying past summer’s high of 142 while still growing.
The acceleration of the crisis is dramatically evident in most parts of the state. According to CDPH, more than 25% of all cases during the health crisis — which was declared a pandemic by the World Health Organization about 40 weeks ago — have come in the past two weeks for California.
That percentage holds roughly true in Los Angeles, the state’s largest county; in Sacramento, home to the state’s capital; in more suburban counties, like Placer; and in harder-hit Bay Area counties, like Contra Costa and Santa Clara.
Areas that were largely spared in earlier surges have been ravaged by the current one. Nevada County, home to 100,000 people in the foothills, has recorded 25 COVID-19 deaths in December after suffering just nine total from March through November. In Santa Cruz County, 31 of the 60 all-time virus deaths have come in the past two weeks, state data show.
California has reported more than 1.72 million lab-confirmed cases of COVID-19 and 21,860 deaths to date, including a record-smashing 379 fatalities on Thursday. It was not immediately clear whether the huge death toll is the result of a backlog. Nearly 140 of the fatalities came from Los Angeles County.
State reports thousands of backlogged cases. Where are those from?
The state health department on Wednesday increased the tally for lab-confirmed COVID-19 cases by nearly 54,000, which would have shattered a single-day reporting record by close to 20,000.
CDPH in statements confirmed this daily case total included a backlog from previous days — initially reported at more than 12,000 infections, with that estimate later revised to 15,337. The true total for Wednesday’s typical reporting period was just over 38,000, still a single-day record but not nearly by the same crushing margin as it had seemed to be.
The state on Thursday reported another head-turning total: 52,281 cases. CDPH said in a news release that the backlog continuing to be cleared made the day’s total “slightly higher” but didn’t give an exact number or estimate. Los Angeles County’s health office reported that it had a backlog of about 7,000 included in its total for the day, all coming from “one large lab.”
If all or most of the backlogged cases are from within the past two weeks, the 14-day average will remain mostly accurate: Wednesday and Thursday’s additions catapulted that rate past 32,000. And in those two weeks, the state reports 11.5% of diagnostic tests returning positive, California’s highest positivity for the entire pandemic.
Ali Bay, communications director for CDPH, in an emailed statement explained the system change that led to Wednesday’s backlog.
“Typically, local public health departments receive cases into an inbox and manually process those cases; however, with high transmission rates, this has become more and more difficult,” Bay wrote. “To support our local public health departments, the state has begun to auto process positive cases for the counties, bypassing the local inbox.
“The data reported (Wednesday) include current auto-processed cases as well as manually processed data from the local health department inbox from several prior days.”
In other words, new lab-confirmed cases were flooding counties’ health offices too heavily for parts of the process that are typically handled manually to continue in that manner, so the state used an “auto process” feature to expedite case reporting. Using that button revealed and reported out about 15,000 infections that had been backed up in counties’ queues.
It’s a different issue from the glitch in early August that blocked disease records from entering the system, creating a backlog. That problem came after a server lost power.
Bay said the new auto-processing feature was added Sunday. It can be turned off in the future, “when the case counts return to lower levels.”
Latest on COVID-19 vaccines: When, who and how many doses?
State and local health leaders have echoed the same metaphor: Safe and highly effective COVID-19 vaccines are the light at the end of the tunnel, but right now we’re still in that tunnel. And given recent case and hospitalization rates, plus the time it will take to manufacture and distribute vaccine doses widely, we may be in that tunnel for at least a few more months.
Even so, developments on the vaccine front continue to offer the best news, if not the only good news at the moment, regarding the coronavirus crisis.
Late last week, the U.S. Food and Drug Administration granted emergency use authorization to a vaccine developed by Pfizer and BioNTech, agreeing that it is safe and about 95% efficient in clinical trials in preventing those who get the shot from contracting the virus.
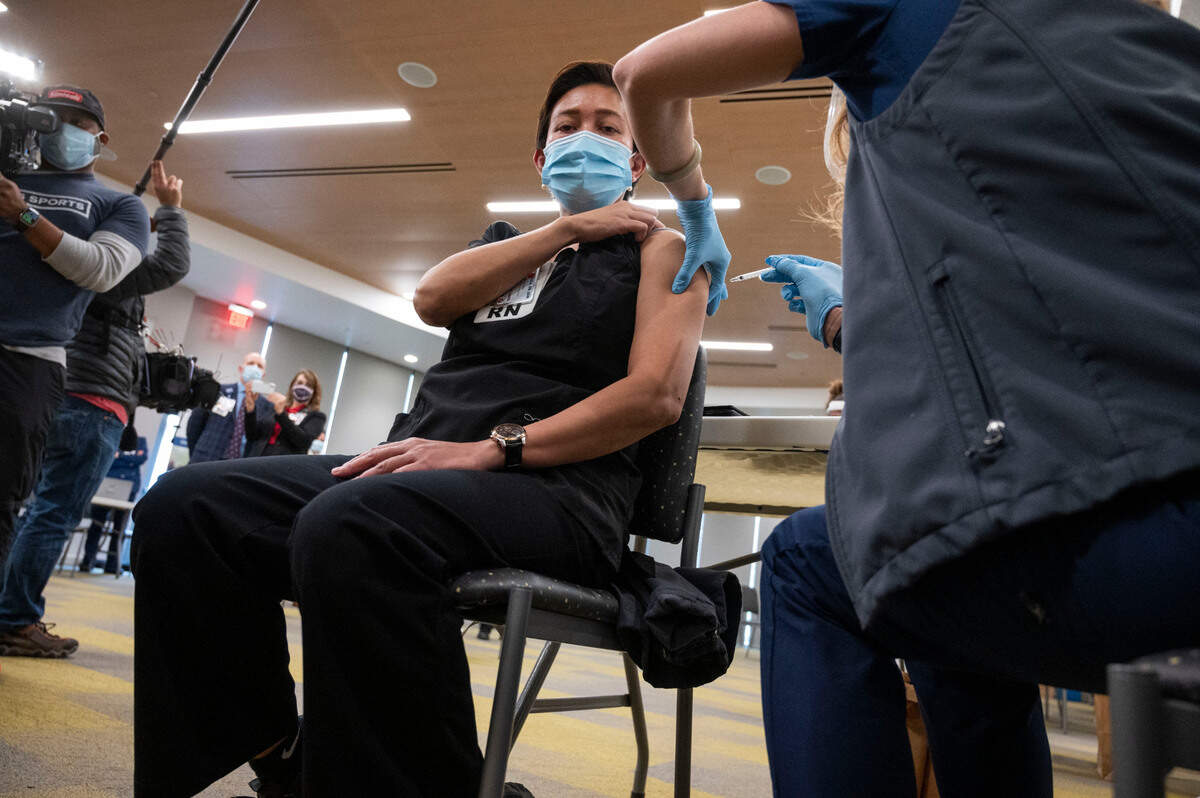
California’s first allocation of 327,000 doses started to arrive Monday and Tuesday. UC Davis Medical Center in downtown Sacramento got its allocation Tuesday morning and began administering the shot to nurses and other health workers.
By Tuesday, Newsom announced the state had secured 393,000 more doses of the Pfizer vaccine, set to come next week.
Today, a key advisory committee is discussing a vaccine candidate by Moderna that uses similar technology to Pfizer’s. The FDA is almost certain to approve Moderna’s vaccine for emergency use within the next couple of days. If it follows the same timeline as that of Pfizer, shots of Moderna’s vaccine could be in Americans’ arms by next Monday.
Newsom has said that between Pfizer, Moderna and others, California is likely to receive more than 2 million doses before the end of the year; Moderna’s first shipment to the state is expected to include more than 650,000. Both the Pfizer and Moderna vaccines are two-dose regimens, which are to be taken about four weeks apart.
California has established that front-line health care workers who handle COVID-19 patients, then nursing and other long-term care home residents, are first in line for the vaccine.
These two groups are being called “Phase 1A.” The state health department hasn’t yet formally announced which population groups will receive the vaccines next, but the expectation is that the other early phases will prioritize additional vulnerable groups, such as health workers not directly involved in COVID-19 patient care, other essential workers and elderly Californians who are not in long-term care homes.
Availability among the general population — the point when anyone who wants one can get one — is expected to take months, possibly not coming until late spring or early summer.
Pfizer’s vaccine has not been approved for children under age 16.
Capital region marching quickly toward 1,000 deaths
Coronavirus activity across the six-county Sacramento area continues to grow exponentially. More than 80,000 residents have tested positive and at least 983 have died of the virus since the start of the health crisis.
Thousands of those infections are still considered active, several hundred are hospitalized and dozens are in intensive care units across Sacramento, El Dorado, Placer, Sutter, Yolo and Yuba counties.
Sacramento County has reported a total of 53,185 infections and 727 related deaths during the pandemic, adding 1,130 cases and 12 deaths Wednesday followed by 1,003 cases and 16 deaths Thursday.
State data showed there were 478 coronavirus patients in Sacramento County hospitals, breaking Tuesday’s record of 473. A staggering 102 were in intensive care, eclipsing the summer peak by 11 patients.
The county maintained 70 ICU beds, down 13 from Wednesday, as hospitals work to balance expanding surge capacity with handling severely sick patients.
County health officials have now confirmed at least 61 virus deaths occurring in the first 13 days of December. Based on preliminary numbers and current hospitalization trends, December’s death toll appears likely to exceed that of November, when at least 133 county residents died. August remains the deadliest month of the pandemic in Sacramento County, at 181 dead.
The county’s latest estimate is that of the 51,000 cases, more than 14,000 are still currently active. That’s a little less than 1% of Sacramento County’s population.
The city of Sacramento has recorded at least 388 virus deaths and nearly 28,000 cases. The latter mark equates to about one in 18 capital city residents having tested positive for the disease.
Yolo County has reported a total of 6,549 infections and 99 deaths. The county confirmed 70 new cases and two fatalities Thursday following 106 cases Wednesday and 110 Tuesday.
The county also reported nine fatalities Tuesday. The local health office in its COVID-19 dashboard said there could be an “influx” of reported deaths in the next few days “as there have been delays in getting confirmation from labs.”
State data updated Thursday showed Yolo with 24 virus patients in hospital beds, down three from the previous day, including 16 in intensive care, down two. Only one ICU bed was available.
Placer County health officials have reported a total of 9,972 infections and 97 deaths, updated Wednesday to add 250 cases and three deaths. The county previously reported one death Tuesday, one on Monday and three last Friday.
State data showed 179 hospitalized, down eight from Wednesday, with a record-tying 27 in ICUs in Placer County.
The state and local hospital dashboards showed Placer with zero ICU beds remaining available on Tuesday; state data showed two available on Wednesday, and Placer on its own dashboard showed one.
The reason for the sudden drop, from 21 beds late last week to zero earlier this week, was not immediately clear, but county health director and interim health officer Dr. Robert Oldham told the Board of Supervisors during Tuesday’s meeting that the ICU capacity metric can vary widely day to day and “does not take into account other beds that can be used for critical care during a surge.”
“So while this is a very serious situation, we want to reassure the public that our hospitals have robust surge plans, are constantly adjusting and can still take care of people,” he said.
El Dorado County has reported 4,412 positive test results and eight deaths. The county added 93 cases Thursday following 121 on Wednesday, 113 on Tuesday and 331 on Monday in a report that included the weekend.
The state on Thursday reported 28 people hospitalized in El Dorado, down four from Wednesday’s record high of 32. Ten were in ICUs, down from 14 three days earlier. Four ICU beds remained available, a decrease by three compared to Wednesday.
In Sutter County, 5,290 people have been infected and 38 have died, with 175 new cases and one fatality reported Wednesday.
Yuba County has reported 3,058 infections and 14 dead, adding 66 new cases on Wednesday.
The bi-county health office dashboard on Wednesday showed 43 Sutter residents hospitalized with 10 in ICUs, plus 16 Yuba residents hospitalized with three in ICUs.
Not all of those 53 are necessarily hospitalized in-county, but Adventist-Rideout on Thursday reported numbers consistent with the above: 53 virus patients were hospitalized there with 13 in ICUs. Two ICU beds remain available.
This story was originally published December 17, 2020 at 8:13 AM with the headline "Coronavirus updates: Southern California ICU capacity hits 0% as state drops to 3%."